Amebiasis is an infectious disease that claims 100,000 lives a year. It can be treated very easily if the necessary drugs are available.
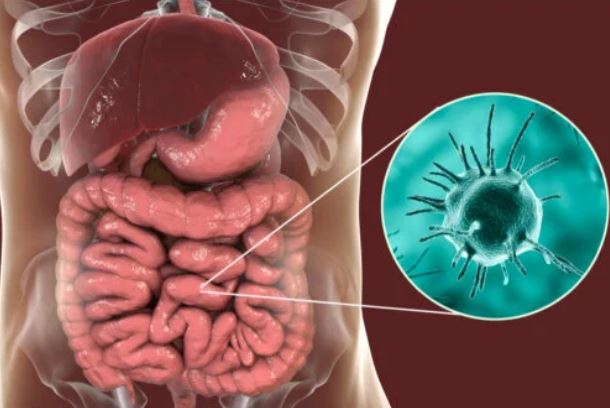
Amebiasis is an intestinal infection caused by the protozoan Entamoeba histolytica, although it can also be caused by Entamoeba dispar and Entamoeba moshkovskii. These microorganisms cause 50 million gastrointestinal cases a year and are responsible for 100,000 deaths annually, especially in hot and tropical climates.
Amebiasis is the third leading cause of death from parasitic diseases worldwide, second only to malaria and schistosomiasis. However, it should be noted that only 1 in 10 infected people end up developing symptoms, from mild diarrhea to bloody stools, dehydration and anemia.
If the Entamoeba infection proliferates and is not treated, the protozoa can enter the bloodstream and travel to other organs, such as the liver, causing an amoebic liver abscess. If you want to know everything about this widespread and multifaceted disease, read on.
What is amebiasis?
As we have said, amebiasis is a very common enteral parasitic infection, since it is estimated that in hot, humid and impoverished regions up to 50% of the population is infected. On the other hand, in industrialized areas with a temperate climate, a very low prevalence is calculated, from 1 to 2% of the population.
According to the Association of Foreign Health Physicians, in low-income countries the infection rate is correlated with the poor level of water sanitation. Almost all infections occur through the fecal-oral route, when the patient comes into contact with contaminated sewage.
On the other hand, it should be noted that all the protozoan species involved in this clinical picture are morphologically identical. The only thing that distinguishes the causative agent Entamoeba histolytica from E. dispar and E. moshkovskii is that the first shows erythrophagocytosis, that is, it can be observed under the microscope how it has ingested red blood cells.
Life cycle of the parasite and causes of contagion
To understand the transmission route of the pathogenic protozoan we must know its life cycle. The Centers for Disease Control and Prevention (CDC) show us Entamoeba’s journey through the human body.
These are the most notable phases of the process:
1.An infected human excretes cysts with his feces. These are the forms of resistance that remain inactive in the environment until they come into contact with a different host.
2.When the new host ingests a cyst (especially with contaminated water), excystation occurs in the small intestine. Here the trophozoites, mobile and active forms that travel to the large intestine, are released.
3.At this point, trophozoites can remain in the intestinal lumen (asymptomatic host), invade the mucosa (intestinal disease), or enter the bloodstream and reach other organs (extraintestinal disease).
4.During the entire duration of the disease, the host will excrete cysts in solid stool and active trophozoites in watery diarrhea. Even so, the only infective variant is cysts, which can survive for days or weeks outside the host.
Thus, cysts often enter the human body through contaminated water. In any case, contagion is not ruled out during sexual intercourse (if the anus is involved). If crops are fertilized with human waste, the chances of an epidemiological outbreak are multiplied.
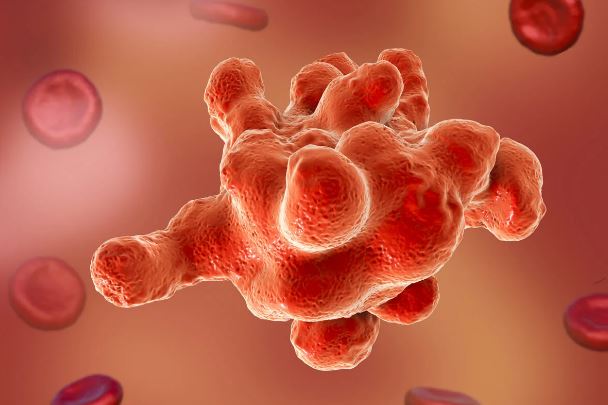
The parasite acquires a cystic form that allows it to survive for long periods in the environment, favoring its spread.
Types of amebiasis
As we have said, 90% of patients do not develop symptoms, since amoebic trophozoites remain in the lumen of the large intestine and do not cause further damage. In the scenario in which signs do occur (1 in 10 infected), 5 variants can be differentiated:
Chronic intestinal amebiasis: slow onset, but long-lasting, characterized by lasting several years, leading to death if not treated. Symptoms of constipation alternate with episodes of diarrhea, bloating and abdominal pain.
Acute intestinal amebiasis: it is the one with the most serious symptoms, lasting from a few weeks to several months. It is characterized by very obvious acute diarrhea, alone or with mucus and blood. If it is not treated quickly the patient is at risk of dehydration.
Toxic amoebic colon: a serious complication. Amoebas perforate the colon and a picture of severe peritonitis occurs, with fever, paleness, decay and hemorrhages within the mucosa of the colon.
Disseminated amoebiasis: amoebae spread from the intestine to other organs. The one that is most often affected is the liver, as protozoa generate abscesses in it.
Intestinal ameboma: it is a granulomatous and proliferative reaction in which a pseudotumor is formed. As indicated in Medigraphic, this rare entity occurs in people who have not been treated and who present bacterial infections secondary to amebiasis.
Main symptoms of amebiasis
According to the United States National Library of Medicine, the most common symptom is diarrhea. This condition occurs when the patient has 3 to 8 stools throughout the day (semi-formed or totally liquid), which can be alone or accompanied by mucus and blood. There are also abdominal cramps and gas (bloating).
Over the days the patient may lose weight, show signs of dehydration, emaciation, and anemia. These clinical signs are common in the chronic variant of the disease, the symptoms of which persist for years if left untreated.
Possible complications
Because diarrhea is made up of water, it is common for the patient to show signs of dehydration in the event of a prolonged period of time, as indicated in the MSD Manual. This state is defined as the loss of body water greater than 3% of the total weight of the patient.
The worst possible scenario is that of systemic involvement by pathogenic protozoa. If amoebas reach the liver, skin, brain, or lungs, the prognosis becomes fatal. Malnutrition and previous pathologies increase the susceptibility to these serious conditions.
Diagnosis of amebiasis
Diagnosis is easy and straightforward: samples are taken from the patient’s stool and analyzed under a microscope. Solid stools contain cysts, while liquid stools harbor trophozoites. In any case, beyond direct observation, genetic sequencing (PCR) methods that search for the amoeba genome are usually necessary.
Amplification of amoebic DNA in the stool is the definitive diagnosis. It is not yet known whether E. dispar causes the disease or not, but it is morphologically identical to E. histolytica. Therefore, it is necessary to go to laboratory techniques that allow distinguishing both organisms.

Direct examination of the stool allows the presence of the parasite to be identified under the microscope.
Treatment
The treatment of choice is an amoebicide taken orally for 7 to 10 days, especially metronidazole. This drug inhibits the synthesis of nucleic acids in protozoa, thereby nipping the infectious mechanism in the bud.
It is dosed at 500 milligrams every 8 hours. If they cannot be ingested orally (by vomiting), they should be given intravenously.
Prevention of amebiasis
Unfortunately, avoiding amoebiasis in a country with poor sanitation is practically impossible. Cysts can survive in the medium for months. The only thing you can do is consume bottled water in the regions where it is endemic.
On the other hand, it should be noted that this table has a very simple treatment, as long as the aforementioned drugs are at hand. Undoubtedly, this pathology is a global health problem linked to socioeconomic status.